Gray's Minithyrotomy
Gray minithyrotomy:
This procedure is named after Steven Gray who along with his colleagues developed this operation in anticipation that some day bioengineered material would become available that can be used to augment the vocal folds. This procedure was designed for access to the subepithelial tissue planes of membranous portion of vocal folds via a small external skin incision placed at the level of vocal fold. The minithyrotomy is made after confirming the level of vocal fold by inserting a 22 number needle on DL scopic visualization.
The needle is inserted at the level of anterior commissure and the position should be confirmed endoscopically. The minithyrotomy is placed 3-5 mm off the midline at the level of vocal fold. A powered 3 mm cutting burr is used to create a tunnel which should be oriented along the long axis of the vocal fold. A strip of fat is gently inserted into this space via the tunnel.
This surgery is performed under general anesthesia. The patient should be intubated with 5.0 (if female) or 5.5 (if male) cuffed endotracheal tube. This small sized tube is preferred because it should not hinder visualization of the vocal folds. The membranous portion of the vocal fold from the anterior commissure to the vocal process of arytenoid cartilage should be clearly visible endoscopically during the entire procedure.
This procedure usually involves dissection of lamina propria along the entire length of membranous portion of the vical fold, edema starts rather early making assessment of the effect of surgery on the table rather difficult. In order to minimize this 10-12 mg decadron is administered intravenously before the start of surgery.
Introduction of laryngoscope:
A suspension laryngoscope is introduced and stabilized in such a way that the entire membranous portion of the vocal folds are clearly visible. The arm of the suspension laryngoscope should also be included in the drape because it could come into contact with the surgeon's gloved hand during the procedure.
The neck is prepared and draped in anticipation of a 2-3cm long horizontal incision overlying the thyroid cartilage. The primary surgeon should be working from the patient's right if right handed and from the left side if left handed.
About 8 - 15 mm long fat strips are harvested from the site of incision.
Visualization of the vocal folds:
The assistant uses a suspension laryngoscope mounted with a 0 degree endoscope to visialize the vocal cords. Pre operative dignosis should be confirmed before the surgery is begun. The tip of the laryngoscope must not interfere with the anatomy of anterior commissure. If placed too distally then the tip can evert the vocal folds and give a false impression of the location of the vibratory margin. The video monitor should be positioned in such a way that it is visible both to the surgeon and the assistant.
Extralaryngeal dissection:
A 2-3 cm horizontal incision is centered over the prow (Adam's apple) of the thyroid cartilage at the anticipated level of vocal folds. As stated earlier fat strips can be harvested. Ideally 1-2 ml of fat is necessary per vocal fold. The fat graft strips should be placed in saline awaiting insertion. Dissection progresses until the strap muscles are encountered. They should be retracted laterally inorder to expose the thyroid cartilage.
Minithyrotomy:
Perichondrial elevation:
The perichondrium covering the thyroid lamina should be elevated after incising it in the midline. Elevation proceeds in a superolateral direction exposing an area of about 1 cm2 on each side of the prow (Adam's apple) of thyroid cartilage.
Needle insertion to localize the level of vocal folds:
A 22 guage needle is passed through the anterior midline of the thyroid cartilage at the anticipated level of the vocal folds. The position of the needle is verified via laryngoscopic vision. This procedure comes with experience. Initially a trial and error may be needed to identify the position of vocal folds. It is advisable to place the localizing needle at the suspected angle and at the level of anterior commissure instead of passing it perpendicular to the thyroid cartilage in the midline.
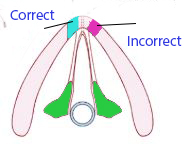
Minithyrotomy is usually centred 3-5 mm off the midline at the level of vocal fold. A 3 mm powered drill is used to create a tunnel through the thyroid cartilage. Once the "give" of penetration through the internal cartilagenous cortex is felt, the drill is withdrawn. A mastoid curette may be used to trim the inside margin of minithyrotomy. It is very important that the minithyrotomy should be oriented along the axis of the vocal folds (somewhat obliquely and not perpendicular to the thyroid lamina).
Entering the correct tissue plane:
Entry into the subepithelial plane is made with a blunt instrument (a probe). The tip of the dissecting instrument should be visible subepithelially when viewed through direct laryngoscope. It is advisable to perform most of the dissection using blunt dissectors of varying dimensions. A Gimmick elevator would suit this purpose. Bellucci scissors can be used to remove severe adhesions.
Creation of an implant pocket:
Surgeon should have a very good idea of the size and shape of implant pocket preoperatively by studying stroboscopic pictures of the patient. Tunnel creation is very crucial and should be done very gently. The implant pocket should be limited as much as possible by the area of pathology. If too large a pocket is created then fat implant could migrate to other areas where it is not needed thereby obviating the effects of surgery.
Complications:
Vocal fold epithelial perforation: In the presence of severe vocal fold scar the vocal fold epithelium could be inadvertantly perforated. Small pinhole perforations do not require the procedure to be abandoned. A larger defect could cause fat extrusion and hence the procedure should be abandoned.
Suboptimal results: Fat implantation via Gray minithyrotomy may not restore normal voice in most cases. This is because fat is not a perfect replacement for altered normal lamina propria tissue. Fat also has a tendency to be reabsored.
Key features of this surgery:
1. It offers access to subepithealial tissues of the vocal folds without the need for mucosal incision.
2. Dissection and fat implantation are performed via neck incision under endoscopic guidance which is advantageous when compared to microlaryngeal techniques.
3. The angle of approach of minithyrotomy allows dissection along the longitudinal axis of the vocal fold and not perpendicular to the thyroid cartilage.
4. This procedure is well suited for rehabilitating patients with sulcus vocalis, and scar conditions associated with superficial lamina propria disturbance.